Are you having trouble sleeping or feeling excessively tired during the day? Numerous prevalent health conditions and Medical Causes of Your Sleep Problems. Discover how to identify whether a medical factor is the culprit behind your nighttime restlessness.
If you’re experiencing poor sleep, there might be an underlying medical reason
Individuals who believe they enjoy restful sleep may still grapple with excessive daytime sleepiness due to various underlying medical conditions. Sleep disturbances can manifest as symptoms of health issues or as side effects of treatments for those problems. The strain of chronic illness itself can lead to insomnia and daytime drowsiness. Common conditions often linked to Medical Causes of Your Sleep Problems encompass heartburn, diabetes, cardiovascular disease, musculoskeletal disorders, kidney disease, mental health issues, neurological disorders, respiratory problems, and thyroid disease. Moreover, various prescription and over-the-counter medications employed to address these health issues and others can compromise the quality and quantity of sleep (refer to the table below).
Chronic physical conditions
Heartburn
Heartburn is often exacerbated when lying down in bed, triggered by the reflux of stomach acid into the esophagus. This issue can be mitigated by avoiding heavy or fatty foods and abstaining from coffee and alcohol in the evening. Utilizing gravity to your benefit, you can elevate your upper body using an under-mattress wedge or blocks positioned under the bedposts. Additionally, there are over-the-counter and prescription medications available that can aid in suppressing stomach acid secretion.
Diabetes
Diabetes, a prevalent and chronic condition characterized by heightened blood glucose levels, arises when cells fail to respond adequately to insulin (a hormone produced by the pancreas), and the pancreas struggles to generate sufficient insulin in reaction. Individuals with poorly controlled blood sugar levels in diabetes may encounter sleep-related issues such as:
- night sweats
- frequent urination
- symptoms of hypoglycemia (low blood sugar)
Moreover, if diabetes has led to nerve damage in the legs, sleep disruptions may occur due to nocturnal movements or pain.
Heart failure
Heart failure, marked by a gradual deterioration in the heart’s pumping function, can lead to the accumulation of fluid in the lungs and tissues. This may cause individuals with heart failure to wake up at night, experiencing breathlessness due to the buildup of extra body fluid around their lungs when lying down. Elevating the upper body with pillows can alleviate this symptom. Some may also encounter a distinct breathing pattern called Cheyne-Stokes respiration, characterized by progressively deep breaths followed by a brief pause in breathing, disrupting their sleep onset.
Benzodiazepine sleep medications prove beneficial for some in maintaining sleep despite this breathing irregularity. Alternatively, others might require supplementary oxygen or a device that increases pressure in the upper airway and chest cavity to facilitate normal breathing and improve sleep.
Men with heart failure often contend with obstructive sleep apnea, a breathing disorder marked by frequent nighttime awakenings. This condition can disturb sleep, induce daytime sleepiness, and exacerbate heart failure. Additionally, individuals with coronary artery disease may experience fluctuations in circadian rhythms, potentially triggering angina (chest pain), arrhythmia (irregular heartbeat), or even a heart attack during sleep.
Musculoskeletal disorders
Arthritis-related pain can pose challenges for individuals trying to initiate sleep and readjust when changing positions Medical Causes of Your Sleep Problems. Moreover, insomnia is a common side effect of steroid treatments. Taking aspirin or a nonsteroidal anti-inflammatory drug (NSAID) just before bedtime may be beneficial in alleviating joint pain and swelling throughout the night.
Those with fibromyalgia, a condition characterized by painful ligaments and tendons, often wake up in the morning still fatigued and experiencing stiffness and discomfort comparable to arthritis. Research examining the sleep patterns of individuals with fibromyalgia reveals that at least half exhibit abnormal deep sleep, characterized by a blend of slow brain waves and waves typically associated with relaxed wakefulness—a phenomenon referred to as alpha-delta sleep.
Kidney disease
Individuals grappling with kidney disease often experience kidneys that have sustained damage to the point where they can no longer efficiently filter fluids, eliminate wastes, and maintain electrolyte balance, as they did when in a healthy state. This condition can lead to the buildup of waste products in the blood, potentially causing insomnia or symptoms akin to restless legs syndrome. Despite undergoing kidney dialysis or transplant, sleep patterns may not always revert to normal, and the reasons for this phenomenon remain unclear.
Nocturia
Nocturia, characterized by the frequent need to urinate during the night, is a prevalent factor contributing to sleep disruption, particularly among older individuals. In mild cases, this condition prompts individuals to awaken at least twice during the night, while severe cases may involve getting up five or six times.
While age is a potential factor in nocturia, other causes encompass various medical conditions (heart failure, diabetes, urinary tract infection, an enlarged prostate, liver failure, multiple sclerosis, sleep apnea), medications (particularly diuretics), and excessive fluid intake post-dinner.
Therapeutic approaches for managing nocturia fall into three categories:
- Addressing and rectifying medical causes.
- Implementing behavioral interventions.
- Utilizing medication.
The initial step involves identifying the root cause and attempting correction. If unsuccessful, behavioral strategies can be employed, such as reducing fluid intake, especially caffeine and alcohol, in the two hours before bedtime. If nocturia persists, doctors may prescribe one of the increasing number of medications approved for treating an overactive bladder.
Thyroid disease
Sleep disruptions can result from an overactive thyroid gland (hyperthyroidism), which excessively stimulates the nervous system, making it challenging to initiate sleep. This condition may also induce night sweats, contributing to nocturnal arousal. Conversely, an underactive thyroid (hypothyroidism) is often characterized by feelings of coldness and increased sleepiness.
Given the thyroid’s influence on various bodily organs and systems, symptoms can be diverse and occasionally perplexing. A straightforward blood test can assess thyroid function. If you observe an array of unexplained symptoms, it is advisable to consult your doctor for a thyroid test.
Breathing problems
Fluctuations in muscle tone around the airways, influenced by circadian rhythms, can lead to nighttime airway constriction, heightening the risk of sudden nocturnal asthma attacks that disrupt sleep.
Challenges in breathing or anxiety about potential attacks may impede the ability to initiate sleep. Additionally, the use of steroids or other respiratory medications with stimulating effects, akin to caffeine, can contribute to this difficulty.
Individuals with emphysema or bronchitis may face sleep difficulties due to increased sputum production, shortness of breath, and persistent coughing.
Medications
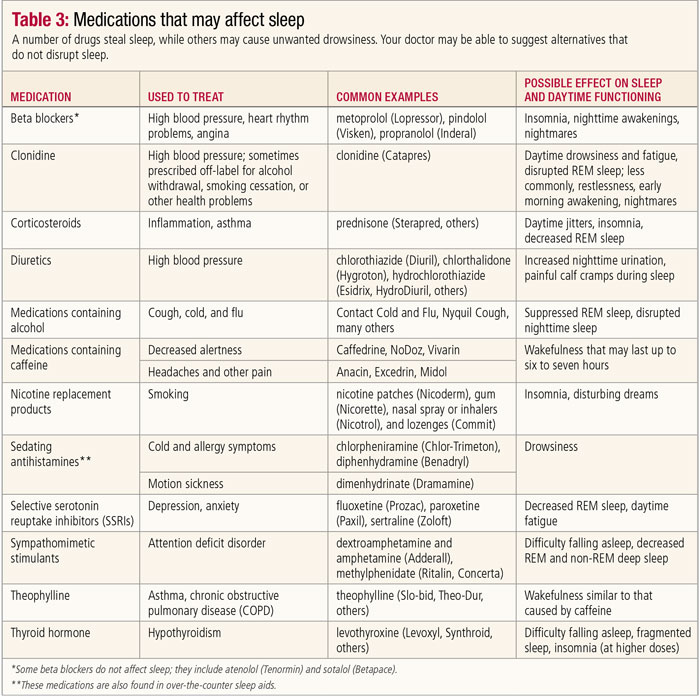
Mental health disorders
Individuals grappling with anxiety or depression commonly encounter challenges in both initiating and maintaining sleep. Consequently, the inability to sleep may intensify the persistent apprehension and stress for some individuals, leading to additional disruptions in their sleep patterns.
General anxiety
Intense anxiety, recognized as generalized anxiety disorder, manifests through persistent, intrusive feelings of concern, unease, or apprehension. These emotions often surpass the typical response to everyday challenges and dangers.
Individuals with generalized anxiety commonly endure heightened, enduring worry daily, spanning six months or longer. Typical symptoms encompass difficulties in both initiating and maintaining sleep, resulting in a sense of restlessness even after sleep.
Phobias and panic attacks
Phobias, characterized by intense fears tied to a specific object or situation, typically do not lead to Medical Causes of Your Sleep Problems unless the phobia is directly related to sleep (such as fearing nightmares or the bedroom itself). Conversely, panic attacks often occur during the night, and the timing of these nocturnal episodes has contributed to the understanding that they have a biological basis.
Sleep-related panic attacks manifest not during dreaming but in stage N2 (light sleep) and stage N3 (deep sleep), which lack psychological triggers. Addressing the underlying issue in many phobias and panic disorders, often with the aid of anti-anxiety medication, may effectively resolve the associated sleep disturbances.
Depression
Given that nearly 90% of individuals grappling with severe depression encounter insomnia, a healthcare professional assessing someone with sleep disturbances will examine depression as a potential factor. Early morning awakening serves as a distinctive feature of depression, and individuals experiencing depression may face challenges falling asleep or contend with restless sleep throughout the night.
In cases of chronic, low-grade depression, also referred to as dysthymia, insomnia or excessive sleepiness could be the predominant symptom. Research conducted in laboratories indicates that individuals dealing with depression tend to spend less time in slow-wave sleep and may rapidly enter REM sleep at the onset of the night.
confusing disorder
Medical Causes of Your Sleep Problems stand out as a notable characteristic of the confusing disorder, also recognized as an excited-depressive illness. Sleep disturbances can intensify excited symptoms, potentially triggering or temporarily alleviating periods of depression. Amid an excited episode, an individual might go without sleep entirely for several days. These episodes are frequently succeeded by a subsequent period of intense fatigue, during which the person may spend the majority of the following days in bed.
Schizophrenia
During the initial and severe stages of a behavior episode, certain individuals may experience minimal sleep. In the periods between episodes, there is a tendency for their sleep patterns to ameliorate, yet it is common for many individuals with schizophrenia to seldom achieve a regular amount of deep sleep.
Neurological disorders
Sleeplessness can be influenced by specific brain and nerve disorders.
Dementia
Sleep regulation and other cognitive functions may be disturbed by Alzheimer’s disease and various forms of dementia. “Sundowning,” characterized by wandering, disorientation, and agitation during the evening and night, can impose significant stress on caregivers, necessitating constant supervision. In such instances, small doses of antipsychotic medications are often more beneficial than benzodiazepine drugs.
Epilepsy
Individuals with epilepsy, a condition characterized by a susceptibility to seizures, are twice as likely to experience insomnia compared to those without the condition. Disturbances in brain waves that lead to seizures may also result in deficiencies in slow-wave sleep or REM sleep. While antiseizure medications may initially induce similar sleep changes, they often rectify these disturbances with prolonged use.
Approximately one in four people with epilepsy encounter seizures predominantly at night, disrupting sleep and causing daytime sleepiness. Sleep deprivation can also act as a trigger for seizures, as observed in college infirmaries during exam periods, where some students experience their first seizures after staying up late to study.
Headaches, strokes, and tumors
Individuals prone to headaches should prioritize avoiding sleep deprivation, as inadequate sleep can contribute to the onset of headaches. Both cluster headaches and migraines may be linked to variations in the size of blood vessels supplying the brain’s cortex, with pain occurring when these blood vessel walls dilate.
Researchers propose that during the body’s compensatory catch-up on lost sleep, it tends to spend more time in delta sleep, a phase when vessels are most constricted. This makes the transition to REM sleep more abrupt, increasing the likelihood of inducing a headache. Headaches that wake individuals up are often migraines, although some migraines can be alleviated by sleep. If accompanied by sleepiness, dizziness, weakness, headache, or vision problems, it may indicate a serious issue like a brain tumor or stroke, necessitating immediate medical attention.
Parkinson’s disease
Using sleeping pills for treatment can be challenging due to the potential exacerbation of Parkinson’s symptoms by certain medications. Some patients taking drugs intended for Parkinson’s treatment may encounter intense nightmares, while others may experience disruptions in REM sleep. Nonetheless, nighttime use of these medications is crucial to preserve the mobility required for changing positions in bed. The incorporation of a bed rail or an overhead bar, commonly referred to as a trapeze, may facilitate movement for individuals with Parkinson’s, potentially enhancing their sleep quality.
Derived with authorization from “Enhancing Sleep: A Guide to Achieving a Restful Night,” a health report published by Harvard Health Publishing.
https://en.wikipedia.org/wiki/Sleep_deprivation




